In Conditions
Follow this topic
Bookmark
Record learning outcomes
The skin, with its own microbiome that balances a careful composition of fungi, viruses and bacteria, not only regulates the body’s temperature but also acts as a protective and waterproof barrier.
It is comprised of three layers:
- Epidermis – the waterproof outer layer. This acts as a barrier and is where the cells that create melanin (pigment) are found
- Dermis – the strong middle layer, which gives the skin elasticity. This is where hair follicles, sweat and oil glands, collagen, elastin, nerves and blood vessels reside
- Hypodermis – the deepest layer, also known as subcutaneous tissue, is primarily made up of fat, which insulates the body, and connective tissue, which attaches the skin to the underlying muscles and bones.
Although the skin works hard, rejuvenating skin cells every 21-28 days, it can face many serious concerns that pharmacy teams can play a significant role in supporting.
“Skin conditions are among the most common reasons people seek advice in community pharmacy,” says Dr Adil Sheraz and Sophia Rajenthiran, spokespeople from the British Skin Foundation.
“From eczema and psoriasis to acne, pharmacy teams are often the first point of contact. Understanding how these conditions differ and how best to support patients can significantly improve outcomes and quality of life.”
So, let’s take a look at some common concerns.
Psoriasis
Psoriasis is thought to affect up to 1.8 million people in the UK, according to the Psoriasis Association. “Psoriasis occurs as the result of an overactive immune system, which then causes symptoms on the skin and can sometimes affect the joints,” explains Amy Ball, communications and engagement lead at the Psoriasis Association.
“When a person has psoriasis, their skin replacement process speeds up, taking just a few days to replace skin cells.”
The condition can occur at any age. However, there are two main peaks when it first occurs – from the late teens to early adulthood and then between the ages of around 50 to 60, Amy explains.
Psoriasis is not contagious and it is not thought to be hereditary, although certain genes have been identified as being linked to the condition. “However,” says Amy, “even if the right combination of genes has been inherited, psoriasis may not appear.”
Let’s take a deep dive into some common groupings of the condition:
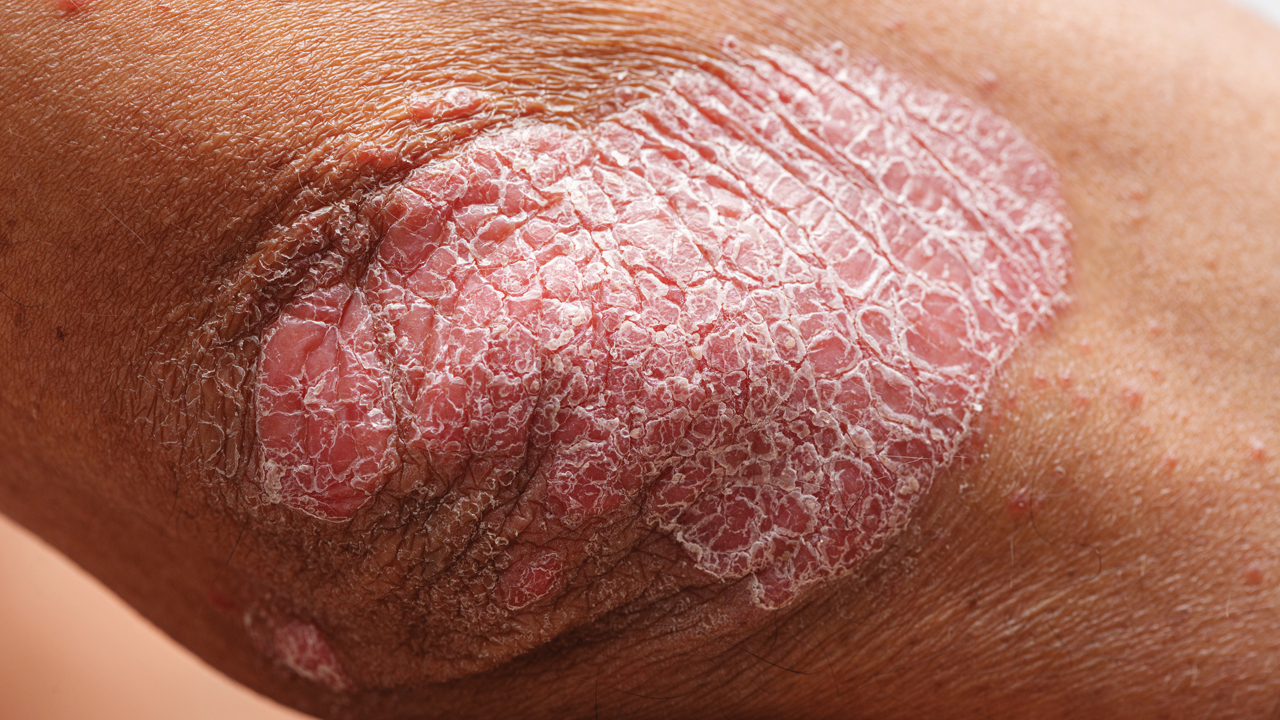
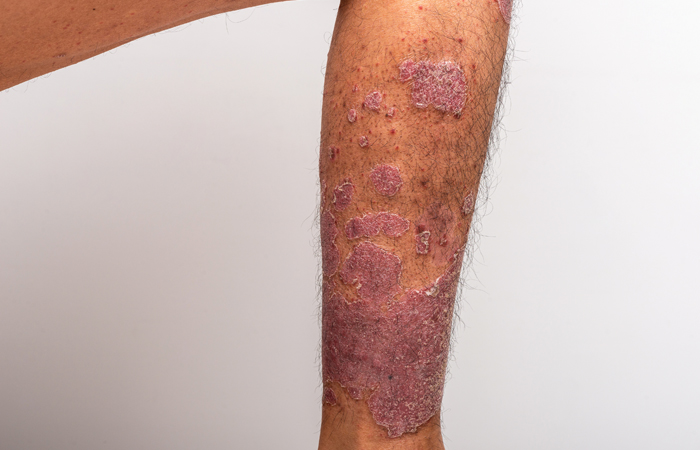
- Plaque psoriasis affects 80 per cent of people with psoriasis, often in conjunction with another form of the condition. Plaques can appear anywhere on the body. A ‘plaque’ is a distinctive physical characteristic of psoriasis – it is a build-up of skin cells that appear as itchy, sometimes painful, silver or white areas.
Depending on the severity of the psoriasis, it can be managed with over-the-counter (OTC) or prescribed topical treatments, including moisturisers and emollients containing ingredients such as vitamin D, coal tar, dithranol or calcineurin.
Topical treatments should be applied gently in the direction of hair growth. “People with psoriasis that does not respond to topical treatments, covers a large area of skin, or is in a high impact site such as the palms of the hands, soles of the feet or face may be referred to a specialist,” explains Amy.
“Specialist treatment can include UV therapy/phototherapy delivered by a dermatologist, systemic treatments (oral tablets to decrease the overactivity in the immune system) or biologics (injections targeting the immune system to reduce inflammation).”
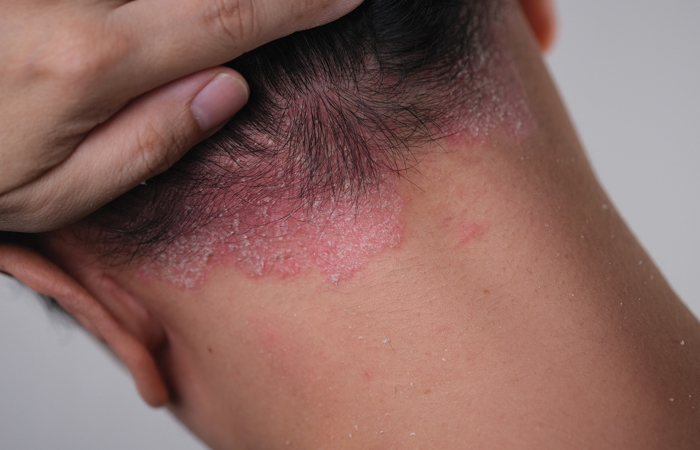
- Scalp psoriasis may be initially misidentified as dandruff as it also creates flaking on the scalp. However, the scalp – as well as in the hairline, ears, neck or forehead – is often the first place that psoriasis appears. Shampoos or scalp applications such as coal tar, salicylic acid, steroids and products containing dithranol are recommended. “It’s important to use treatments as prescribed, even if psoriasis improves, as continuous treatment can help prevent flare-ups and minimise side effects,” says Amy.
Hair should be brushed gently to avoid scratching the scalp.
“Psoriasis is thought to affect up to 1.8 million people in the UK”
- Nail psoriasis affects up to 50 per cent of people with psoriasis, but increases to 80 per cent amongst those who also have psoriatic arthritis (a chronic autoimmune condition affecting some people with psoriasis). Fingernails and/or toenails may be affected. To help identify nail psoriasis, the Psoriasis Association suggests looking for signs of:
- A nail that has lost its shape
- Discolouration
- Small dents on the nail surface (also known as pitting)
- Nails that split or break easily
- Thickening of the nails
- Onycholysis – nails lifting from the nail bed.
The main treatment for nail psoriasis is steroid-based. However, this is not suitable for long-term use. Those
who are affected should try to avoid damaging or injuring their nails to prevent the spread to healthy nails or the condition worsening.
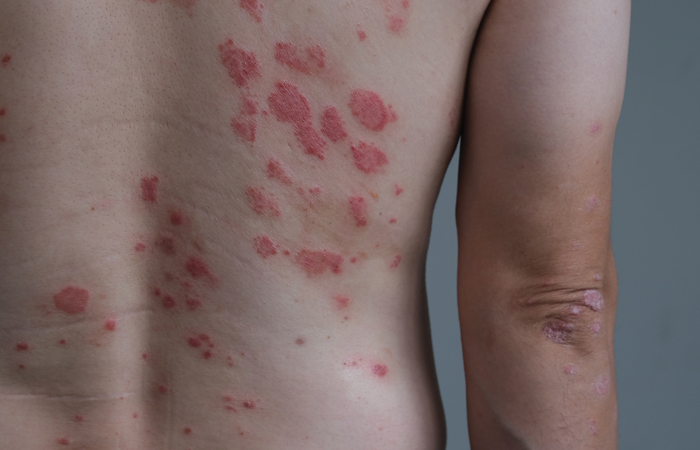
- Guttate psoriasis, often known as ‘tear’ or ‘raindrop’ psoriasis, manifests as a widespread rash, often across the torso. The spots are usually 1cm in size and appear as a brighter pink colour on lighter skin or darker patches on darker skin. “It can occur at any age, but is most common amongst children, adolescents and younger adults,” says Amy.
Guttate psoriasis often occurs after a bout of streptococcal throat infection. If someone is prone to this infection, they may be affected by repeated bouts of guttate psoriasis.
“It usually clears up after several weeks or months, depending on how quickly treatment is started. Some people may continue to have flares from time to time, or find it evolves into one of the other types of psoriasis,” Amy explains.
As with plaque psoriasis, topical treatment is used to treat guttate psoriasis if it has not cleared up on its own. New treatments should be reviewed every four weeks for adults and every two weeks for children. UV light therapy may be suggested for more persistent cases.
Recognition aid
Red flags
Knowing when to refer urgent cases of psoriasis is just as important as knowing how to recognise and recommend treatment options. Some key signs that require urgent referral include:
- Rapidly worsening or spreading psoriasis
- Redness with severe pain, hot skin or swelling
- A high temperature, chills or feeling unwell with psoriasis
- Pus-filled blisters
- Discolouration of plaques (e.g. presenting as yellow or green)
- Facial swelling and breathing difficulty.
“If psoriasis is particularly widespread or severe, or if it is in an area which has a high impact on day-to-day life (such as the hands, feet, face or genitals) then specialist care may be needed,” explains Amy Ball, communications and engagement lead at the Psoriasis Association.
The mental toll
Due to the trial-and-error nature of psoriasis treatment, sufferers can become incredibly frustrated and demotivated. This may potentially impact their mental health.
“Many things can be disrupted by psoriasis, from work to relationships, getting a good night’s sleep or deciding what to wear,” explains Amy.
“Some may feel distressed or anxious about their skin and may decide to cover it up, either with clothing or special skin camouflage make-up, while others are comfortable not covering their psoriasis at all.”
The Psoriasis Association runs a confidential helpline service to provide information and signposting to further support. “This helps people to navigate the variety of psoriasis types and treatments, which can at times feel overwhelming,” explains Amy.
“Our forums are also a popular source of community and knowledge-sharing, which helps people to feel less alone.”
“Skin conditions are more than ‘just skin deep’,” add Dr Sheraz and Sophia. “With the right knowledge, pharmacy teams can play a vital role in early recognition, appropriate management, and holistic patient support. Empathy, clear advice, and timely referral can make a lasting difference not only to skin, but to confidence and wellbeing.”
For customers looking for further support for their psoriasis, pharmacy teams can signpost them to the Psoriasis Association (psoriasis-association.org.uk) and the British Skin Foundation (britishskinfoundation.org.uk).
“Empathy, clear advice, and timely referral can make a lasting difference”
Adressing acne
Diagnoses of acne have risen globally since 1990, according to a study published in the British Journal of Dermatology, which suggested that a whopping 95 per cent of adolescents are affected in the UK.
Acne often occurs on the face and neck but it can also be found on the back and chest. “In simple terms, the skin becomes oily, pores become blocked, bacteria grow, and inflammation leads to spots,” say Dr Adil Sheraz and Sophia Rajenthiran, spokespeople from the British Skin Foundation.
Other contributing causes include environmental factors, diet, hormones and genetics.
Acne can have different levels of severity:
- Mild – characterised by comedones (small bumps) and a few spots
- Moderate – with inflammatory papules and pustules
- Severe – particularly where there are nodules or a risk of scarring.
Because acne can be very visible, it’s emotional impact can be intense. In fact, according to Acne Support, as many as one in four people who have acne will experience a change in their mental state.
Key treatment principles include treating early to prevent scarring, combining treatments for better efficacy, and managing expectations because improvement typically takes six to 12 weeks.
In addition, those with acne should avoid scrubbing or over-washing their skin and avoid touching, picking or squeezing spots as this can lead to scarring.
People should “be cautious with social media skincare trends”, warn Dr Sheraz and Sophia. Instead, if customers ask for help with their acne and OTC treatments haven’t helped, refer them to the pharmacist who will be able to explain further treatment options.
Skin camouflage products may help, especially if acne has left scars or is making someone feel really self-conscious. To find out if a skin camouflage clinic is available in your area, visit changingfaces.org.uk. For more information, customers can also be signposted to The British Skin Foundation (britishskinfoundation.org.uk) and Acne Support (acnesupport.org.uk).
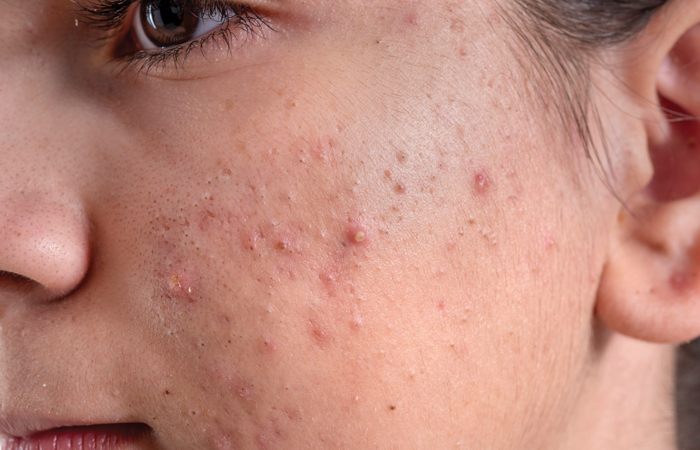
Acne sufferers should avoid picking or popping spots as this can lead to scarring.
All about eczema
Eczema affects six million people in the UK. This common skin condition can sometimes be misidentified as psoriasis and vice versa, so it’s important to be able to recognise the difference between the two.
Firstly, consider the physical appearance of the condition and be sure to pay attention to notable differences.
“Eczema typically presents with dry, itchy, inflamed skin, and commonly affects flexures such as the inside of the elbows and behind the knees. The skin may appear cracked, weepy, or crusted during flares,” explain Dr Sheraz and Sophia.
“In contrast, psoriasis presents as well-demarcated, thick plaques with silvery scale and commonly affects extensor surfaces such as the elbows, knees, and scalp. It is usually less itchy than eczema but may involve nail changes and joint symptoms.”
The second thing to note is the cause. While eczema is often associated with asthma and hayfever, it is caused by a skin barrier defect and immune hypersensitivity. Common triggers for eczema can include allergies, cold weather, stress and clothing.
On the other hand, Amy explains: “Psoriasis is triggered by changes in the immune system that cause it to become overactive. This could include streptococcal throat infections, physical and emotional stress, certain medications, excessive alcohol consumption or the site of injury to the skin (which is known as the Koebner phenomenon).”
Treatment for eczema focuses on repairing the skin’s barrier and inflammation, whereas treatment for psoriasis aims to slow skin cell turnover and targets immune pathways.
For eczema, emollients are first line and should be applied “frequently throughout the day to hydrate and protect the skin,” explain Dr Sheraz and Sophia.
“Topical corticosteroids are used during flares to reduce inflammation, with potency tailored to the site and severity of symptoms.”
Pharmacy teams can share lifestyle advice with eczema sufferers. “Patients should be advised to use emollients regularly, even when the skin is clear, avoid harsh soaps and fragranced products, and keep showers short and lukewarm,” say Dr Sheraz and Sophia.
“Treatments should be applied in the correct order, and adherence is key, as many treatments fail due to underuse.”
It is also important for those using steroids to protect their skin from UV harm by covering up in the sun.
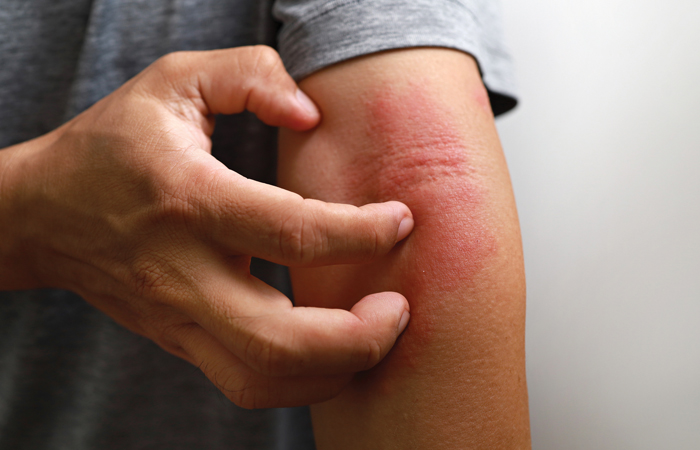
Eczema does not appear with the same silvery plaques as psoriasis.